Understanding the Unique Challenges of Treating Comorbid OCD and ASD (Autism Spectrum Disorder) with ERP
How OCD Presents Differently in Individuals with ASD
In typical OCD, compulsions are primarily performed to neutralize distressing thoughts and relieve uncertainty. However, in individuals with both OCD and ASD, compulsions often stem from a need to restore a black-and-white, rule-based and often inflexible understanding of the world.
Rather than seeking to alleviate anxiety, they are striving to maintain a rigid sense of order and correctness.
Patients with OCD/ASD do not experience fear in the same way as those with traditional OCD. Instead, their discomfort stems from rigid, literal thinking. A patient with comorbid ASD and OCD may not engage in compulsions due to fear that something bad will happen or to relieve uncertainty. Rather, they feel compelled to follow strict, inflexible beliefs about how they 'must' act or think. While their behaviors may resemble OCD, the underlying motivation is different.
The distress driving their compulsions is more akin to the discomfort experienced by someone with ASD when their structured routines or worldview are disrupted, rather than the uncertainty and anxiety that typically characterize OCD.
The Role of Inflexibility and Rule-based thinking in Comorbid OCD and ASD
The DSM-5 criteria for ASD include: "Insistence on sameness, inflexible adherence to routines, or ritualized patterns of verbal or nonverbal behavior (e.g., extreme distress at small changes, difficulties with transitions, rigid thinking patterns, greeting rituals, need to take the same route or eat the same food every day)."
For individuals with both OCD and ASD, compulsions often serve to reinforce this rigid structure rather than to alleviate uncertainty.
In short, triggers make them uncomfortable, but they aren't scared…
This means that traditional Exposure and Response Prevention (ERP) therapy—the gold standard treatment for OCD—may not be as effective if it focuses solely on habituation and learning to live with uncertainty and doubt.
Adjusting ERP for Comorbid OCD and ASD
Traditional ERP is designed to help individuals tolerate the discomfort of uncertainty, doubt and anxiety. However, when treating comorbid OCD and ASD, ERP must be adapted. If compulsions are driven by rigid thinking rather than anxiety, treatment can be more effective if there is an additional focus on developing flexibility and helping individuals adopt a more nuanced and adaptable worldview.
In this context, treatment should go beyond mere exposure to doubt, distressing thoughts or situations. Instead, it should include modifying the rigid rules the individual has created.
A significant part of therapy involves teaching individuals to see more "gray" in their world and to tolerate the discomfort they experience when things don’t align with their rigid, black-and-white framework.
The goal of exposure is not simply to help them live with anxiety and doubt, but to help them navigate the discomfort of being flexible—learning to act and view the world in a more adaptable, nuanced way.
Example: The Role of Rabbinic/Clergy Involvement
This is particularly important when treating scrupulosity/religious OCD.
Typically, when treating scrupulosity, clinicians often minimize Rabbinic involvement to avoid reinforcing reassurance-seeking behaviors. However, in cases where OCD is entangled with ASD-driven rigidity, Rabbinic input can be beneficial.
Since the individual’s compulsions may stem from an inflexible, rule-based worldview, a trusted authority (Rav) can play a crucial role in helping to rewrite the 'rules' in a way that aligns with reality and religious law (Halacha).
This external validation helps the patient recalibrate their rigid beliefs, allowing them to function more adaptively. Once these new guidelines are established, ERP can then help them tolerate the discomfort of following rules that may feel counterintuitive to their rigid thinking.
Conclusion
Treating comorbid OCD and ASD requires a nuanced approach that goes beyond traditional ERP. I find that ERP can be enhanced when adapted to address the rigid thinking patterns associated with ASD. By focusing on the discomfort of flexibility, clinicians can help individuals reshape their worldview in a way that reduces distress and promotes functional living.
Written by Eliyahu Serkez
The Anxiety & OCD Therapy Practice
Share
Tweet
Share
Mail

By Eliyahu Serkez
•
April 3, 2025
What is OCD? Obsessive-compulsive disorder (OCD) is a mental health condition that affects millions of people worldwide. It involves two key components: 1. Obsessions – Intrusive, repetitive and unwanted thoughts, images, or urges that cause significant distress. 2. Compulsions – Repetitive behaviors or mental acts performed to reduce the distress caused by obsessions or to prevent a feared event. For example, someone with OCD may fear that they will get sick from germs (obsession) and compulsively wash their hands for hours each day (compulsion) to relieve their anxiety. While compulsions may provide short-term relief, they ultimately make OCD worse, strengthening the cycle over time. How the Vicious Cycle of OCD Begins and Continues The Natural Response to Pain To understand why OCD is so persistent, it helps to compare it to physical pain. Imagine touching a hot stove—your instinctive reaction is to pull your hand away. This response is automatic and protective, helping you avoid harm. Similarly, when people with OCD experience distressing thoughts, they instinctively try to "pull away" from them by performing compulsions. However, unlike touching a hot stove, where avoiding the heat prevents injury, avoiding distressing thoughts through compulsions only strengthens the cycle. The thoughts always come back… The Brain’s Role in Reinforcing OCD OCD tricks the brain into thinking that avoidance is necessary for safety. Two key mechanisms drive this process: 1. Avoidance reinforces the perception of danger – When we repeatedly avoid something, our brain starts to categorize it as dangerous. We don’t avoid things unless they pose a real threat, right? The brain applies the same logic to OCD thoughts, reinforcing the false belief that they are dangerous and must be avoided. 2. Increased sensitivity to triggers – Once the brain labels something as dangerous, it becomes hyper-aware of it. The more an individual avoids or reacts to an obsession, the stronger and more distressing it becomes over time.
By Eliyahu Serkez
•
March 7, 2025
Imagine sitting down for dinner, and the sound of someone chewing makes your skin crawl. Your heart races, your fists clench, and you feel an overwhelming urge to escape or lash out. This isn’t just a mild annoyance—it’s a condition known as misophonia. What is Misophonia? Misophonia is an intense emotional reaction to specific sounds, often repetitive noises made by other people. Common triggers include: • Chewing, slurping, sipping • Pen clicking, foot tapping, keyboard typing • Sniffing, breathing, or throat clearing For people with misophonia, these sounds don’t just cause irritation—they can trigger frustration, rage, anxiety, or panic, making social interactions and everyday life incredibly difficult. Why Does Misophonia Happen? Misophonia isn’t just about sound sensitivity; it involves psychological, emotional, and behavioral factors. Researchers propose that misophonia develops due to a combination of personality traits, learned responses, and psychological conditioning: 1. Personality Traits: ○ Many individuals with misophonia tend to have perfectionistic or rigid personalities. ○ They have a strong need for order and control, making unexpected or repetitive sounds feel unbearable. 2. Learned Associations (Classical Conditioning): ○ A person might initially feel frustrated with a family member for an unrelated reason. ○ If that person makes a specific sound (e.g., chewing loudly), the brain associates the sound with frustration. ○ Over time, the sound alone triggers an automatic emotional response. 3. Avoidance and Reinforcement (Operant Conditioning): ○ To escape the discomfort, people with misophonia may avoid meals, wear headphones, or isolate themselves. ○ While avoidance provides temporary relief, it actually reinforces the brain’s sensitivity to trigger sounds, making the problem worse. 4. Hypervigilance: ○ Misophonia sufferers often become hyper-aware of trigger sounds, constantly anticipating and dreading them. ○ This heightened state of alertness leads to even more distress. A New Approach to Treating Misophonia: EASE EASE (Experiential Acceptance and Stimulus Engagement), is a therapy that addresses these factors and helps sufferers change their relationship with trigger sounds rather than trying to eliminate them. The treatment has three main steps: 1. Ending Toxic Hope • Many misophonia sufferers hold on to the hope that other people will stop making the sounds. • This “toxic hope” fuels frustration and makes them feel trapped. • Therapy helps individuals accept that trigger sounds are a part of life and that focusing on changing others is unhelpful. • Letting go of the idea that others "should" stop making trigger sounds is crucial for acceptance. • A technique called “victorious surrender” is used, where individuals imagine themselves as powerless against the sound, which paradoxically reduces emotional resistance. 2. Reducing Avoidance • Avoiding trigger sounds only makes sensitivity worse. • Treatment encourages people to gradually expose themselves to triggers in a controlled way. • Identifying and eliminating different forms of avoidance, such as physical (leaving the room), cognitive (trying to ignore it), and social (asking others to stop), is essential. 3. Stimulus Engagement • Instead of fearing and avoiding sounds, individuals are guided to engage with them mindfully. Why EASE Works • Breaks the avoidance cycle: Avoidance reinforces sensitivity to sounds, so gradual exposure helps rewire emotional responses. • Reduces emotional resistance: By eliminating toxic hope and control strategies, sufferers can let go of the fight against sounds. • Encourages acceptance: Acceptance of discomfort, rather than resistance, leads to long-term improvement in tolerance. • Addresses underlying personality traits: The focus on reducing perfectionism and rigidity allows for greater flexibility in responding to triggers. Final Thoughts: Can Misophonia Be Managed? While misophonia can feel isolating and overwhelming, research suggests that it can be managed with psychological interventions. The key is not to fight or avoid trigger sounds but to change the way the brain responds to them. By focusing on acceptance, reducing avoidance, and mindful engagement, people with misophonia can reclaim their quality of life. You’re not alone, and help is available.

By Eliyahu Serkez
•
February 21, 2025
"Learn why Misokinesia—an intense aversion to certain movements—often worsens over time and how avoidance fuels the cycle. Learn about the brain’s role in reinforcing triggers and explore EASE therapy, a powerful treatment approach to breaking free from Misokinesia’s grip.

By Eliyahu Serkez
•
February 20, 2025
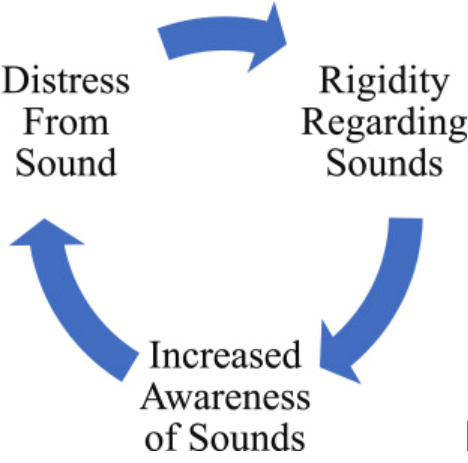
Is misophonia a type of OCD, and can ERP (Exposure and Response Prevention) help? While misophonia and OCD share similarities—such as distressing triggers and compulsive responses—their core emotional drivers differ. OCD is rooted in fear of future consequences, while misophonia stems from frustration with present discomfort. Understanding these distinctions is key to effective treatment. Learn why ERP may not be the best approach for misophonia and explore alternative therapies like EASE (Experiential Acceptance and Stimulus Engagement) for lasting relief.
By Eliyahu Serkez
•
February 18, 2025
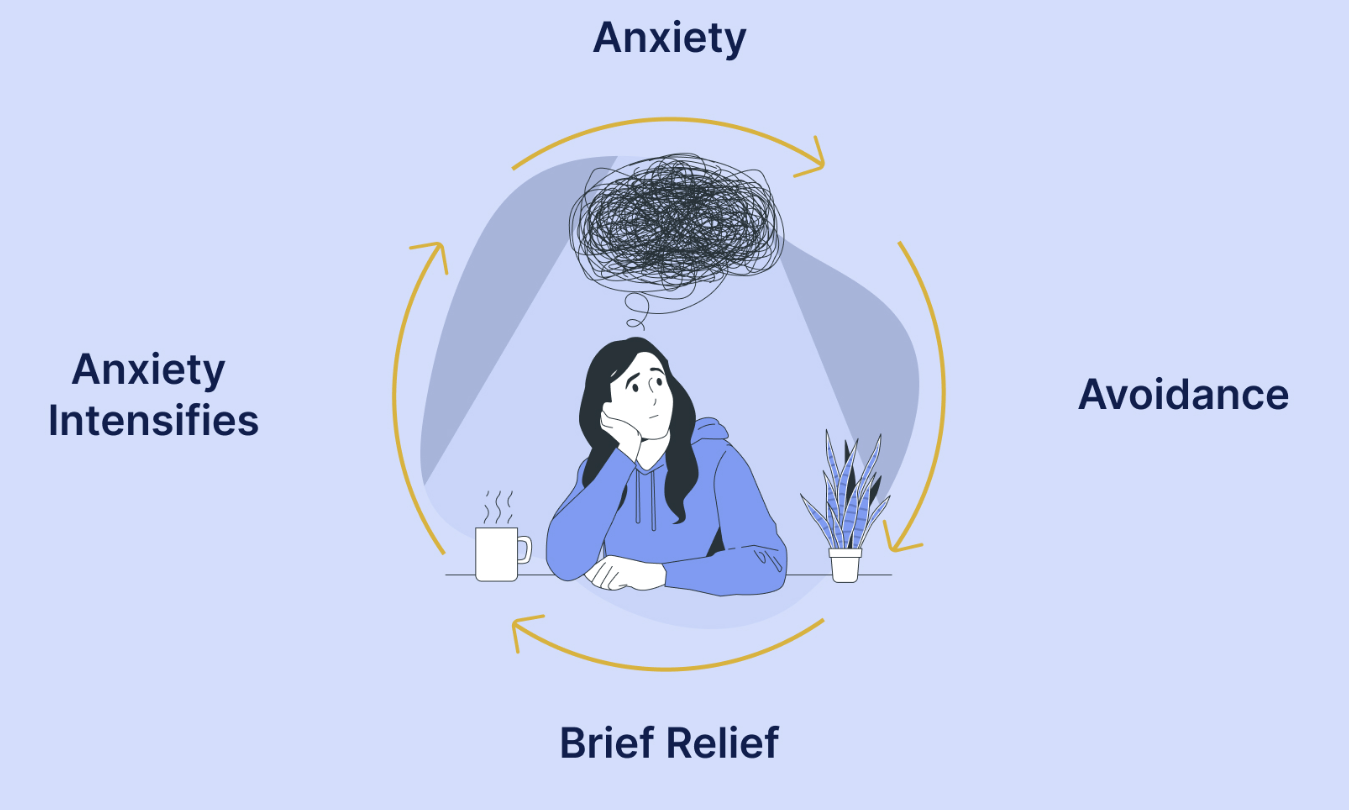
Misophonia creates a vicious cycle of avoidance and heightened sensitivity to sound. Learn why traditional coping methods fail and why misophonia seems to get worse with time. Discover how EASE therapy can break this cycle, offering lasting relief. Understand how misophonia affects the brain and find hope in overcoming sound triggers for a more peaceful life.
By Eliyahu Serkez
•
February 13, 2025
Learn about the self-perpetuating cycle of anxiety and OCD, where intrusive thoughts lead to compulsions that reinforce fear - keeping people trapped with their thoughts. Learn how why the OCD thoughts keep coming back. Exposure and Response Prevention (ERP) therapy disrupts this cycle by helping individuals face their anxiety without engaging in compulsive behaviors, offering effective relief and long-term management strategies for both anxiety and OCD.

By Eliyahu Serkez
•
January 26, 2025
Learn about the link between emetophobia and OCD, including common symptoms and how Exposure and Response Prevention (ERP) therapy can be used to treat both. This structured approach helps individuals confront their fear of vomiting gradually, reducing anxiety and improving quality of life. Learn how therapy treatment for emetophobia works.

By Eliyahu Serkez
•
January 17, 2025
Discover how Exposure and Response Prevention (ERP) therapy can help you overcome OCD. Learn what ERP is, how it works, and why it's the gold standard treatment for reducing obsessive thoughts and compulsive behaviors. Find out if ERP will work for you and how motivation plays a key role in success. Start your journey to a life free from OCD with proven techniques that gradually reduce anxiety without compulsions.
Interested to learn more? We’re here to help!
The Anxiety & OCD
Therapy Practice
We specialize in treating all forms of Anxiety, OCD & Misophonia
Find us on:
Psychology Today: https://www.psychologytoday.com/profile/1156406
Locations
New Hempstead, NY
Ramsey, NJ
Howell, NJ
Telehealth-Virtual
