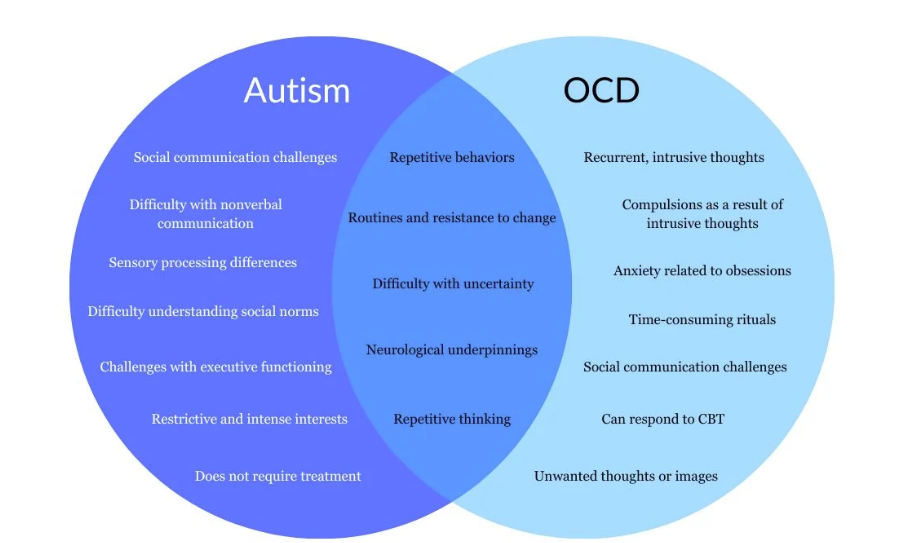
Obsessive-Compulsive Disorder (OCD) is typically understood as a condition in which individuals engage in compulsions to relieve anxiety and doubt. However, when OCD coexists with Autism Spectrum Disorder (ASD), the underlying motivations for engaging in compulsions can be quite different. Understanding these differences is crucial for tailoring treatment approaches effectively.
How OCD Presents Differently in Individuals with ASD
In typical OCD, compulsions are primarily performed to neutralize distressing thoughts and relieve uncertainty. However, in individuals with both OCD and ASD, compulsions often stem from a need to restore a black-and-white, rule-based and often inflexible understanding of the world.
Rather than seeking to alleviate anxiety, they are striving to maintain a rigid sense of order and correctness.
Patients with OCD/ASD do not experience fear in the same way as those with traditional OCD. Instead, their discomfort stems from rigid, literal thinking. A patient with comorbid ASD and OCD may not engage in compulsions due to fear that something bad will happen or to relieve uncertainty. Rather, they feel compelled to follow strict, inflexible beliefs about how they 'must' act or think. While their behaviors may resemble OCD, the underlying motivation is different.
The distress driving their compulsions is more akin to the discomfort experienced by someone with ASD when their structured routines or worldview are disrupted, rather than the uncertainty and anxiety that typically characterize OCD.
The Role of Inflexibility and Rule-based thinking in Comorbid OCD and ASD
The DSM-5 criteria for ASD include: "Insistence on sameness, inflexible adherence to routines, or ritualized patterns of verbal or nonverbal behavior (e.g., extreme distress at small changes, difficulties with transitions, rigid thinking patterns, greeting rituals, need to take the same route or eat the same food every day)."
For individuals with both OCD and ASD, compulsions often serve to reinforce this rigid structure rather than to alleviate uncertainty.
In short, triggers make them uncomfortable, but they aren't scared…
This means that traditional Exposure and Response Prevention (ERP) therapy—the gold standard treatment for OCD—may not be as effective if it focuses solely on habituation and learning to live with uncertainty and doubt.
Adjusting ERP for Comorbid OCD and ASD
Traditional ERP is designed to help individuals tolerate the discomfort of uncertainty, doubt and anxiety. However, when treating comorbid OCD and ASD, ERP must be adapted. If compulsions are driven by rigid thinking rather than anxiety, treatment can be more effective if there is an additional focus on developing flexibility and helping individuals adopt a more nuanced and adaptable worldview.
In this context, treatment should go beyond mere exposure to doubt, distressing thoughts or situations. Instead, it should include modifying the rigid rules the individual has created.
A significant part of therapy involves teaching individuals to see more "gray" in their world and to tolerate the discomfort they experience when things don’t align with their rigid, black-and-white framework.
The goal of exposure is not simply to help them live with anxiety and doubt, but to help them navigate the discomfort of being flexible—learning to act and view the world in a more adaptable, nuanced way.
Example: The Role of Rabbinic/Clergy Involvement
This is particularly important when treating scrupulosity/religious OCD.
Typically, when treating scrupulosity, clinicians often minimize Rabbinic involvement to avoid reinforcing reassurance-seeking behaviors. However, in cases where OCD is entangled with ASD-driven rigidity, Rabbinic input can be beneficial.
Since the individual’s compulsions may stem from an inflexible, rule-based worldview, a trusted authority (Rav) can play a crucial role in helping to rewrite the 'rules' in a way that aligns with reality and religious law (Halacha).
This external validation helps the patient recalibrate their rigid beliefs, allowing them to function more adaptively. Once these new guidelines are established, ERP can then help them tolerate the discomfort of following rules that may feel counterintuitive to their rigid thinking.
Conclusion
Treating comorbid OCD and ASD requires a nuanced approach that goes beyond traditional ERP. I find that ERP can be enhanced when adapted to address the rigid thinking patterns associated with ASD. By focusing on the discomfort of flexibility, clinicians can help individuals reshape their worldview in a way that reduces distress and promotes functional living.
Interested to learn more? We’re here to help!
The Anxiety & OCD
Therapy Practice
We specialize in treating all forms of Anxiety, OCD & Misophonia
Find us on:
Psychology Today: https://www.psychologytoday.com/profile/1156406
Locations
New Hempstead, NY
Ramsey, NJ
Howell, NJ
Telehealth-Virtual
